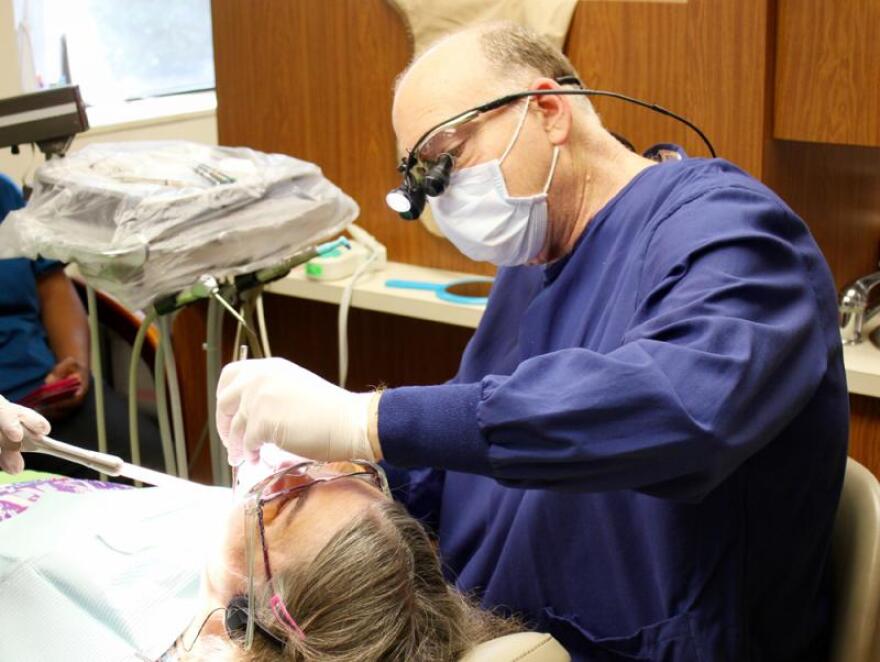
Legislators in cash-strapped Kansas approved a 4 percent cut to Medicaid reimbursements this year. That’s made an already tough situation even tougher for a dentist in Prairie Village who serves some of the state’s most vulnerable residents.
John Fasbinder’s dental office was busy on a recent Tuesday.
Three employees helped in the reception area, answering phones and clicking away at computers. Hygienists tended to patients in three dental chairs in the main clinic. Fasbinder and his associate, Seth Cohen, flitted among those patients and others in private rooms set up for more intensive work.
Most days are like this for Fasbinder. At his Prairie Village office, he takes patients on Medicaid — no matter how old they are, what part of Kansas they come from or how difficult they are to treat.
That’s rare. In fact, Fasbinder thinks he may be the only oral surgeon left in the state who takes all comers.
“I try hard to get dentists to see Medicaid patients, and a lot of them won’t,” he said.
That’s because Kansas Medicaid, or KanCare, pays about 40 cents on the dollar compared to private insurance for dental work. And that was before legislators and Gov. Sam Brownback cut the reimbursements another 4 percent this year to help close persistent budget holes.
Fasbinder said that will make it even harder to convince his colleagues to take Medicaid patients.
“To take money away from a system that’s already compensating so little is not the answer,” he said. “And maybe we do need to be speaking to those representatives … that may be very well-meaning, but whoever’s pulling on their coattails or trouser legs is speaking stronger than we are. We need to let them know — logically, rationally, the best we can — that this is not working.”
Rates trending down
Medicaid reimbursement rates for dental care have dropped steadily in Kansas for years.
In 2003, reimbursements for Kansas children were among the top 10 in the nation, covering almost 70 percent of what private insurance would pay. By 2013 Kansas had dropped to the middle of the pack, with reimbursements around 47 percent of private pay. The reimbursements for treating adults are even less competitive.
Kevin Robertson, executive director of the Kansas Dental Association, said most of the state’s oral surgeons will see Medicaid patients up to age 21. Some take older adults who live in their counties and “a few will treat on a case-by-case basis.”
But he agreed that it is challenging to get any Kansas dentist to treat the thousands of adults covered by Medicaid, including about 7,700 who have intellectual or developmental disabilities.
“The lack of an increase in provider rates for 15 years has created a climate where the number of oral surgeons that accept Medicaid is low,” Robertson said via email. “The upcoming 4 percent decrease in provider rates will not make that any easier.”
John Fales, a pediatric dentist in Olathe and the president of the dental association, submitted written testimony about the reimbursement cuts to federal officials who hosted a Medicaid forum in Salina last month.
Fales said he has provided dental care to children and adults with special needs on Medicaid since 1983 and he has always done so at a loss because the reimbursements didn't cover expenses. The cuts will increase the losses by thousands of dollars.
"A 4 percent decrease in reimbursement will likely be the death knell for KanCare’s ability to provide local access to dental care for these patients without an adequate number of dental providers," Fales wrote.
Tight budgets a challenge
Kansas legislators have been dealing with tight budgets in the wake of large income tax cuts spearheaded in 2012 by Gov. Sam Brownback and Republican leaders.
Increases to Medicaid reimbursements aren’t likely without a change in tax policy or a sudden spurt of dramatic economic growth.
Legislators this year pushed through a bill to give health providers continuing education credits in exchange for charity care, as an incentive for more uncompensated care.
But Fasbinder said he’s already doing as much of that as he can, for people who don’t even have Medicaid.
“We get a lot of patients sent to us that don’t have anything,” he said. “From Catholic Charities, from abuse places. The prosecuting attorney’s office has called us about people who have been beat up. And we try to take care of everybody we can.
“There’s not always funding. But you know what? It’s just a ‘gotta do’ thing. I would like to get better funding from the state. I would like to see them better take care of the money that they’re taking taxes out for me and everybody else.”
Fasbinder said that if legislators think all dentists are living large, they’re mistaken. He drives a 2008 Toyota Camry.
That’s his choice, he said. He could be making more money if he shifted his patient mix to serve more patients with private insurance.
But some of Kansas’ most medically fragile people are on Medicaid, and Fasbinder is worried about them not getting care.
“There’s a lot of people whose needs are not getting met, and they’re not paying us just wonderful amounts,” Fasbinder said. “It’s making it hard for us to survive. We have trouble with access to care, and we’ve got trouble with meeting the needs.”
Focus on the patients
Fasbinder said he thinks legislators would make Medicaid reimbursements a higher priority if they just met some of his patients.
Patients like Sarah Matthies.
Matthies has a disability, the result of a serious back injury she suffered while horseback riding. She had another dentist who treated Medicaid patients. Then she was hospitalized for several months. When she got out, she knew she was behind on her dental care, with four cavities and a busted crown. So she tried to see her dentist.

“Then I get a letter saying he’s retiring and I go, ‘Darn,’” Matthies said, “and the dentist who took over is not taking Medicaid.”
At first Matthies wasn’t sure where she would turn. Eventually she found Fasbinder through a website run by the state Medicaid contractor who handles her case.
“It was real hard to find Dr. Fasbinder, and he’s quite a ways away,” said Matthies, who lives in Olathe.
Matthies has to arrange transportation to her dental appointments at least three but no more than 30 days in advance. But at least she lives in the same county as Fasbinder’s practice.
Many of his other Medicaid patients travel much farther, and some have far more severe disabilities. Some are developmentally disabled, or nonverbal, and find routine dental work traumatic. Parents rave about how Fasbinder treats their special needs children.
“Let me just tell you, I’m probably going to get emotional here,” Jennifer Smith said in a phone interview. “He is extremely compassionate and very patient.”
Smith is executive director of the Autism Society of the Heartland and has two grown children who have autism. She has witnessed Fasbinder treating nonverbal patients by holding their hands while he works and talking them through what he’s doing because he can tell they are in pain even if they can’t describe the pain for him.
“He is treating that person as a person, an individual,” Smith said. “Not talking over them.”
Smith said she and others also go to Fasbinder because he is a licensed anesthesiologist who will do sedation dentistry even at Medicaid rates. That’s very rare, and often it’s the only practical way to do dental procedures on patients with intellectual or developmental disabilities.
“(For) so many of our loved ones with disabilities, it’s a sensory issue,” Smith said. “They’re not understanding what’s going on, and having to sit and have someone poke and prod in their mouth — it’s difficult.”
Smith, who lives in Gardner, said she was disappointed to hear that the Medicaid reimbursements are being reduced. Many people in the autism community would struggle to find dental care without Fasbinder, she said.
“He has them come from all over because of what he does,” Smith said. “When you’re a family that has a loved one with a disability and you find a provider that spends the time and, even if there’s an emergency, will schedule something to immediately get them in, you want to stay with them because they get it.”
A matter of life and death
Anne Hull has two adult sons who have developmental disabilities and go to Fasbinder’s clinic. She knows it’s challenging for providers like Fasbinder to run a business on what Medicaid pays and finds the recent reductions to reimbursements alarming.
Hull wonders if the general public understands how many of their fellow Kansans have developmental disabilities and how dental pain can affect their ability to thrive.
“As a country, we need to make sure that people who truly need the help get it,” Hull said. “And that they’re not suffering in pain.”

Fasbinder said doing the sedation dentistry for his patients with developmental and intellectual disabilities is a moral obligation, but not easy on the bottom line.
“It’s tough when they go to sleep and we’ve got to do everything Medicaid allows me to do on them at the time and make those treatment decisions without a lot of information that I can garner ahead of time because I can’t get near them,” Fasbinder said. “I won’t get in their mouths (before they’re sedated). I can’t get in their mouths — nobody can — to try to figure out the best therapy, the best treatment, for them.”
There are many restrictions on what dental work Medicaid will cover, especially for adults. For example, tooth extractions are only covered when deemed medically necessary. That makes dentists even more reluctant to take Medicaid patients.
Fasbinder said some of the patients he sees have been without dental care so long, extractions aren’t just medically necessary — they’re a matter of life and death.
“The truth is it’s killing people,” Fasbinder said. “The truth is there are more hospital admissions than we’ve had in a long time for dental. Ask the emergency docs what they can do for that. Nothing. Nothing. Because they don’t have a lot of dentists on staff. They can (only) throw antibiotics and pain pills at them, which increases our world resistance to antibiotics, and we’re all going to pay for that eventually.”
Fasbinder is 61. He plans to continue practicing another 10 to 15 years, while handing off ownership of his clinic to Cohen. Before he retires, Fasbinder would like to see a stronger provider network for Medicaid patients.
Fasbinder wishes his colleagues would take more Medicaid patients with complex medical conditions and developmental and intellectual disabilities. But he doesn’t entirely blame them for not doing so. It’s a shared societal responsibility, he said, and the current Medicaid rates represent a societal failure.
“There’s got to be ways we can take care of these folks,” Fasbinder said. “We’re supposed to. The federal government mandates that we’re supposed to. Our ethical values mandate we’re supposed to take care of these people.”